Data-driven Healthcare
July 10, 2022

Welcome to the New Normal. These are the latest words entering the vocabularies of Americans as we enter the new phase post-pandemic. It has opened a heated conversation on “holistic healthcare” and how data can drive this. Over the last few decades, healthcare entities have been accumulating heaps of data to run the day-to-day activities in silos but never really emphasized turning data into insights. The divergent disease and economic modeling we have seen during the pandemic make it clear that data is helpful, but insights are what saves lives. We know that failure points in the continuum of healthcare are costly. A prescription goes unfilled, or a patient missing a follow-up appointment — these are everyday occurrences. But which oversight will cost more if not corrected?Advisory Board research shows that 15%-35% of patients are at “rising risk” — that is, they are becoming sicker and more expensive in invisible ways.
The patient’s symptoms aren’t severe enough to require interaction with a primary care physician; they may even be seeing specialists, but an underlying systemic health issue is undetected. Eventually, 18% of the rising-risk patients will become high-risk (i.e., much sicker and more expensive), finally drawing a response from today’s reactive system. The generated data about the rising patient may have been accurate, but the insight tying it all together was lacking. Proactive insights and intervention are staples of value-based health care.
A welcome development from the pandemic is that telehealth has finally found its feet, overcoming longstanding barriers, resistance, and inertia. In the past, skeptics have argued there wasn’t enough data to prove the effectiveness of telehealth/telemedicine. One health plan executive recently noted we are during a national experiment.
Just as tech-shy families and friends have leaped to connecting virtually during the pandemic, they have embraced virtual healthcare. With cross-state barriers lifted and multiple regulatory waivers issued during the emergency, providers also have flocked to telehealth and telemedicine.
The million-dollar question is – will telehealth/telemedicine resolves all the issues we have in the patient’s care continuum?
The obvious answer is NO. Only when we start gathering more real-time data and creating actionable insights on top of it is when we can bring in a visible change to the otherwise stale healthcare.Digital data may offer some solutions. For instance, it may help doctors find better treatment for chronic diseases, which now contribute to about 75% of total US healthcare spending. Data will also help to provide more proactive care to the members in the face of shrinking numbers of healthcare providers. The American Medical Association expects a shortfall of between 46,900 and 121,900 physicians by 2032 in the US. Healthcare data gets generated internally and externally. Only when data, used holistically, data analysis can improve healthcare prediction, disease prevention and personalization of healthcare.
We have come a long way in generating high-quality data about patients thanks to many digital initiatives in the last couple of decades. Meanwhile, patients themselves can create and monitor their health data using wearable technologies.
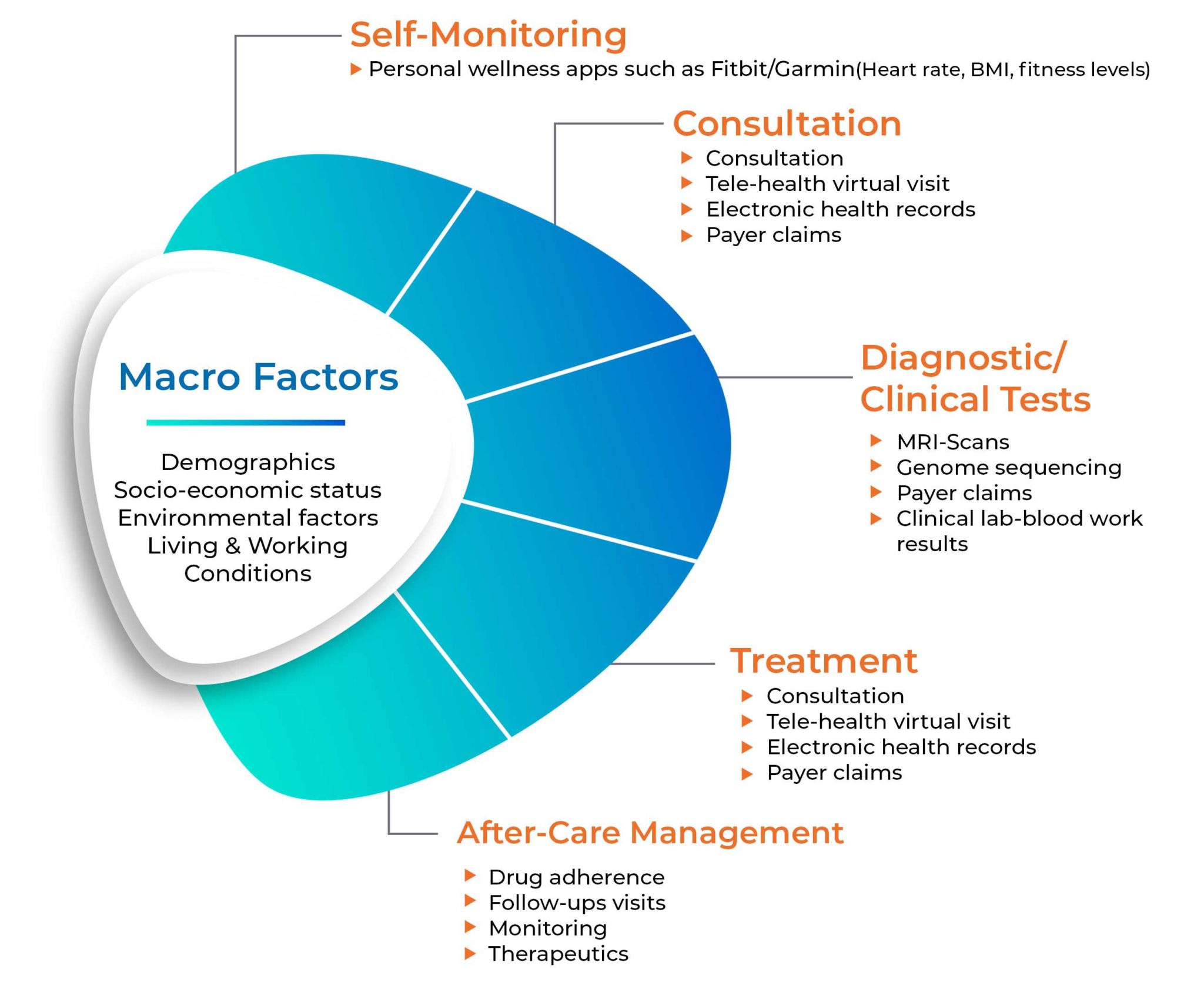
The data collected outside of the healthcare realm also needs to be considered for a holistic view. For example, SDoH will play a pivotal role in understanding patient risks. External datasets, coupled with healthcare analytics are used to understand the healthcare trends and stratify population risks.
Data Analytics and Insights
Some tidbits on the volume of data getting generated in US healthcare –
- 2013 – 153 exabytes
- 2017 – 700 exabytes
- 2020 – 2,314 exabytes
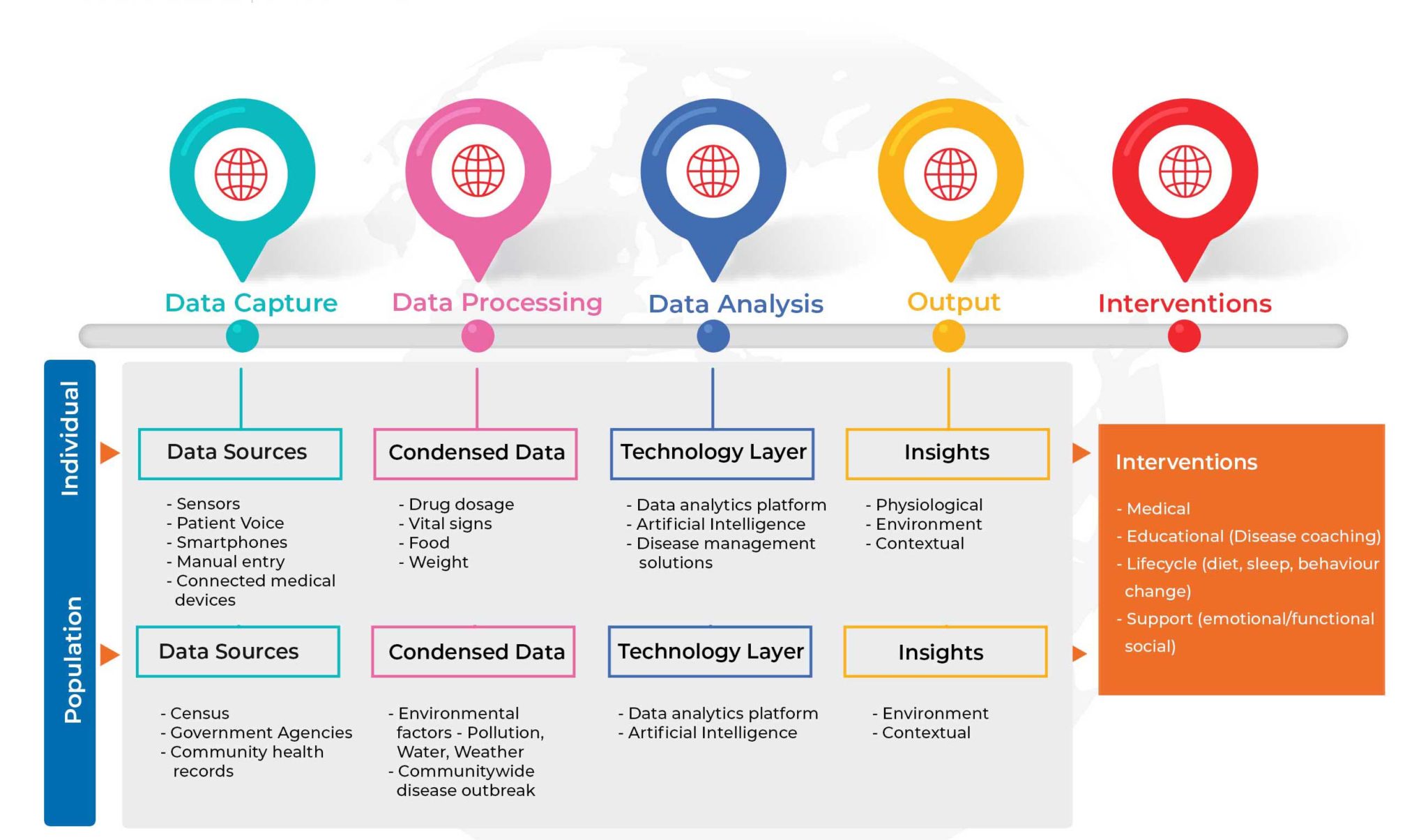
Below figure depicts the data accumulation from different sources and how at the end they converge at the end to provide insights to members.